Practice of Medicine
article
Reducing the Risks of Postpartum Hemorrhage
Postpartum hemorrhages account for 4% of medical malpractice claims among OB/GYN physicians insured by MagMutual. In fact, postpartum hemorrhage is considered an obstetric emergency and among the top five causes of maternal mortality in developed nations.1
To help OB/GYN doctors reduce the incidence of postpartum hemorrhage, MagMutual’s medical faculty and risk consultants have analyzed our claims data, determined the main causes of claims related to postpartum hemorrhage and developed strategies to improve patient outcomes.
Top Risks
The main causes of claims related to postpartum hemorrhage are:
- Failure to diagnose post-operative bleeding
- Failure to recognize a complication of treatment
- Failure to properly respond
Top Strategies for Reduction
Based on these top risk drivers, implementing the following clinical and operational strategies can help you prevent unexpected outcomes and increase defensibility of a medical malpractice claim:
Clinical strategies
- Prior to delivery/procedure, type and cross a blood sample and notify the blood bank if excessive blood loss is anticipated. After a vaginal or Cesarean delivery, always anticipate a postpartum hemorrhage (PPH), especially if labor is prolonged since muscle fatigue can occur. Also consider PPH if a patient has the signs/symptoms of chorioamnionitis (as infection is the primary cause of PPH) or if a patient had a previous PPH.
- When bleeding occurs, keep in mind that actual blood volume loss is often more than your visual impression, and if the patient becomes hypotensive, transfuse immediately. If bleeding persists despite massage, oxytocin, methergine or carboprost (Hemabate), or if the patient develops tachycardia, pallor or nausea, prepare for the OR. Absent rapid improvement, do not delay going to OR for D&C and possible laparotomy. Consult with MFM regarding the need for progesterone therapy in continued cervical management.
Familiarize yourself with the methods and use of intrauterine balloon tamponade. You must be able to place a Bakri (or similar) balloon for tamponade. Likewise, be familiar with operative techniques such as uterine compression sutures to avoid hysterectomy. Consider uterine artery embolization by interventional radiology.
Operational strategies
- Establish a process and have the equipment to accurately measure blood loss. This ideally should be a routine procedure on the maternity ward, according to current evidence.
- Ensure that the department has a readily available postpartum hemorrhage cart and designated team members to assist in an emergency. Call for assistance from anesthesia and a back-up OB provider early if PPH does not resolve at bedside. Utilize your hospital's protocols, rapid response code and rapid transfusion protocols.
Other Top Risks
Postpartum hemorrhage is among the most severe claims against OB/GYNs according to our data, but we’ve also identified several other drivers of loss based on claims frequency:
Risk Drivers by Top Cause
| Key Loss Driver | Top Clinical Loss Cause | Top Non-Clinical Contributing Factor | % of Claims |
|---|---|---|---|
| (A) Neonatal injury following shoulder dystocia | Procedural | Documentation | 10% |
| (B) Ureter injury during hysterectomy | Procedural | Documentation | 7% |
| (C) Failure/delay in performance of C-section | Procedural | Communication | 7% |
| (D) Bowel perforation during GYN surgery | Procedural | Communication | 6% |
| (E) Medication error | Treatment | Communication | 5% |
| (F) Postpartum hemorrhage | Treatment | Clinical Systems | 4% |
Risk Drivers by Frequency
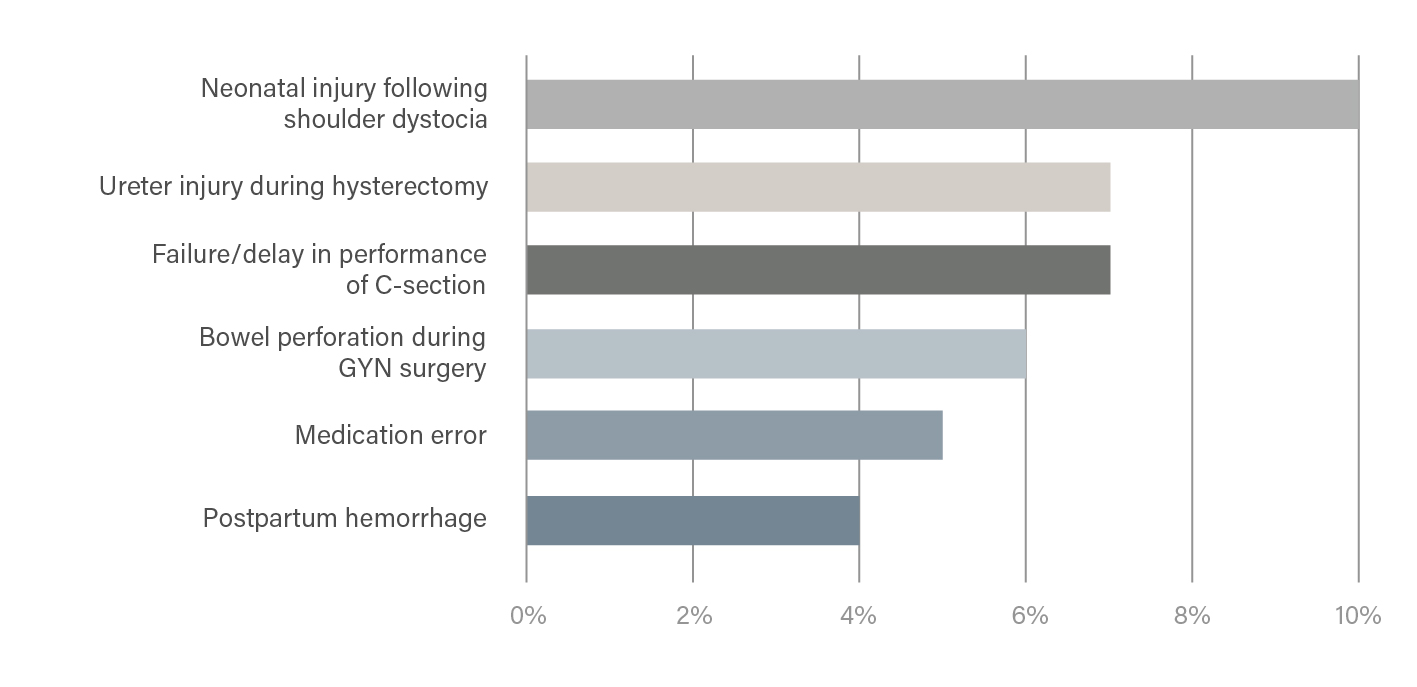
Download the full report with indemnity payment information and strategies for all the key loss drivers to help you reduce risk in the top areas that claims occur.
MagMutual PolicyOwners: Log in to view the full report
Not a policyholder? Download Here
Data Collection & Methodology
Data is based on MagMutual closed claims from 2011-2021 and corresponding exposure data. Clinical and non-clinical loss drivers are based on an in-depth review of each claim by a medical professional or clinical risk consultant. Risk reduction strategies are based on input from practicing physicians.
[1] https://www.uptodate.com/contents/overview-of-postpartum-hemorrhage">https://www.uptodate.com/contents/overview-of-postpartum-hemorrhage
03/24
Disclaimer
The information provided in this resource does not constitute legal, medical or any other professional advice, nor does it establish a standard of care. This resource has been created as an aid to you in your practice. The ultimate decision on how to use the information provided rests solely with you, the PolicyOwner.